How to Stop Stomach Burning Immediately: Fast Relief That Actually Works
That fire in your belly is not waiting for you to schedule a doctor’s appointment. Here are the remedies that work right now — ranked by how fast they act — along with what is probably causing it and when it is time to take the burning more seriously.
Do This Right Now
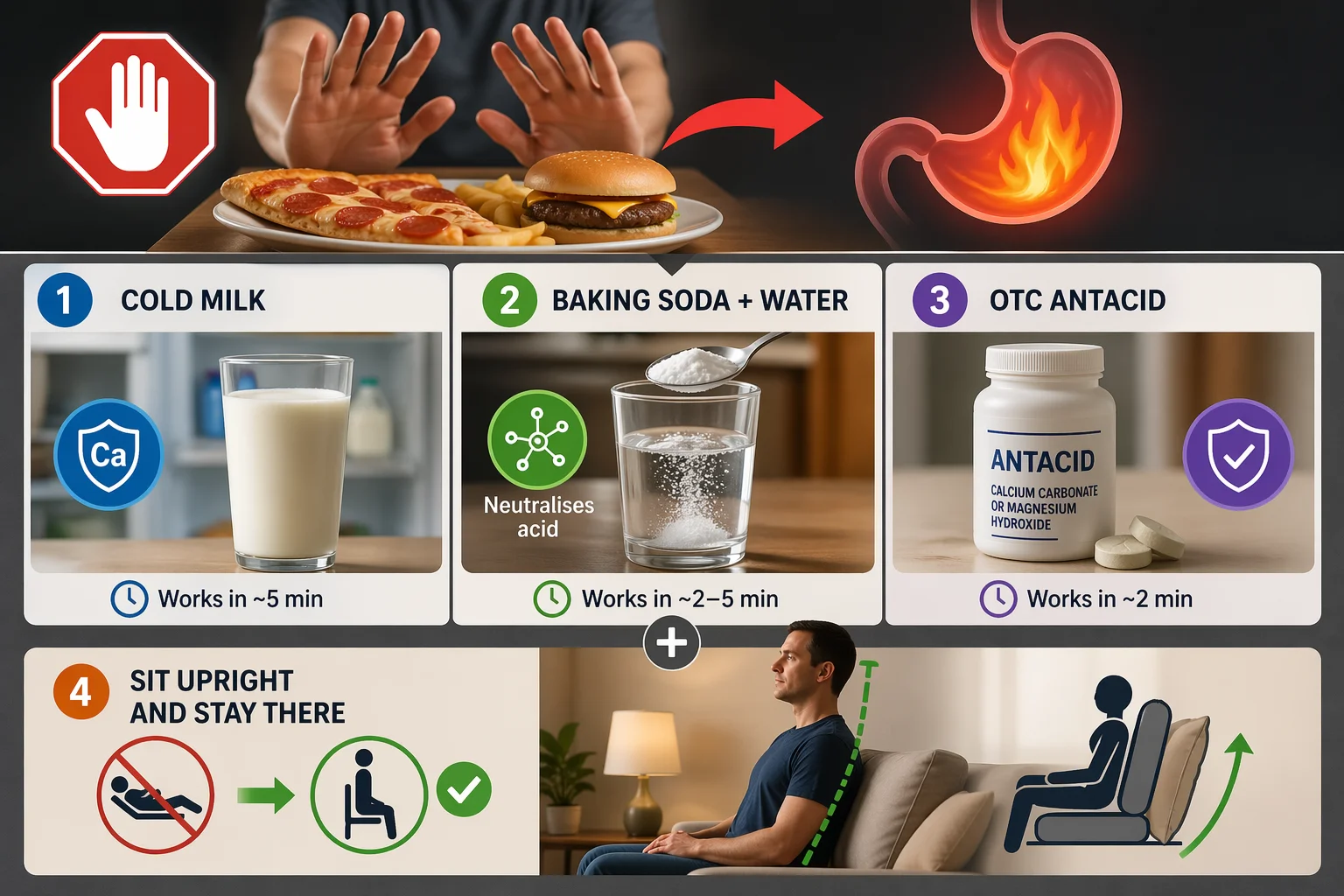
Before anything else — stop eating. Whatever is in front of you, push it aside. Adding more food to an already irritated stomach adds fuel to the fire, regardless of what that food is.
Then pick one of these three options depending on what you have available:
For most people, an OTC antacid or baking soda in water provides the fastest relief — usually within 2 to 5 minutes. Cold milk and coconut water are gentler and take a little longer. All of these work by neutralising stomach acid or coating the stomach lining to reduce irritation. They treat the symptom, not the cause — which is why understanding what triggered it matters.
Why Your Stomach Is Burning
Stomach burning is not a single condition — it is a symptom that several different things can produce. What you do about it, and how worried you should be, depends on which of these is most likely driving it in your case.
Kitchen Remedies That Work — and a Few That Do Not Always
Your kitchen probably already has several things that can help. Here is what the evidence actually supports, including honest notes on the ones that work for some people but not all.
| Remedy | How It Helps | How to Use It | Caution |
|---|---|---|---|
| Cold Milk | Calcium neutralises acid; cold temperature soothes lining | One glass, sipped slowly | Generally Safe |
| Baking Soda | Direct antacid — neutralises acid on contact | ½ tsp in a full glass of water | Occasional Use Only |
| Ginger Tea | Anti-inflammatory; reduces nausea and acid irritation | Fresh slices steeped 10 min in hot water | Generally Safe |
| Chamomile Tea | Relaxes digestive tract muscles; reduces inflammation | One cup, warm not boiling | Generally Safe |
| Coconut Water | Naturally alkaline; cools and soothes gut lining | One cup, plain and unsweetened | Generally Safe |
| Banana | Alkaline pH; forms a light protective coating on stomach lining | One ripe banana, eaten slowly | Generally Safe |
| Fennel Seeds | Antispasmodic; reduces gas, bloating, and acid buildup | 1 tsp chewed after eating or steeped as tea | Generally Safe |
| Aloe Vera Juice | Anti-inflammatory; may soothe stomach lining | Half a cup of pure, unsweetened juice | Buy from trusted source only |
| Apple Cider Vinegar | May help balance stomach pH for some people | 1 tbsp diluted in a glass of water before meals | Works for some, worsens for others |
| Peppermint Tea | Cooling and antispasmodic for mild indigestion | One cup, warm | Avoid if you have acid reflux — relaxes sphincter |
Peppermint appears on almost every “stomach burning remedies” list online, and it genuinely helps with some types of indigestion. However, if your burning is caused by acid reflux or GERD, peppermint relaxes the lower oesophageal sphincter — the exact valve that is already failing to keep acid in your stomach. For acid reflux patients, peppermint can make things noticeably worse. If you are unsure which type of burning you have, skip it.
Over-the-Counter Options
Home remedies are effective for mild, occasional burning. When the burning is more intense or the home options are not cutting it, OTC medications are both faster and more reliable. There are three categories worth knowing about.
Stop Doing These Things Right Now
Some of what makes stomach burning worse is not what you eat — it is what you do in the hour after eating. These specific behaviours directly worsen acid reflux and burning, and stopping them costs nothing.
- Lying down or reclining within 2 to 3 hours of eating — gravity keeps acid in the stomach; lose it and acid travels upward
- Wearing tight clothing around your waist — this increases pressure on the stomach and pushes acid up
- Drinking coffee, alcohol, or citrus juice while experiencing burning — all three directly increase acid production or relax the sphincter
- Eating again to try to soothe the burning — more food means more acid production
- Taking ibuprofen or aspirin for the pain — NSAIDs irritate the stomach lining and will worsen the burning
- Smoking — nicotine weakens the lower oesophageal sphincter and significantly worsens acid reflux
- Drinking large quantities of water all at once — small sips are fine; a large volume increases stomach pressure
Preventing It From Coming Back
If this is happening more than occasionally, the remedies above are treating the symptom while the cause continues. These are the changes that address what is actually generating the burning — not just what quiets it in the moment.
Large meals are one of the most direct triggers for acid production and reflux. Your stomach physically expands under pressure, the sphincter gets stressed, and acid finds its way up. Eating four to five smaller meals across the day instead of two or three large ones reduces that pressure consistently. According to Medical News Today, portion control is among the most evidence-backed lifestyle changes for reducing chronic stomach burning.
Stomach burning triggers are personal. Spicy food is a universal culprit for many, but coffee triggers it for some people while being fine for others. Tomatoes, chocolate, onions, garlic, and mint are common triggers that most people never identify because they never connect the meal to the burning 30 minutes later. A simple food diary for two weeks — noting what you ate and when burning occurred — can identify your specific triggers with surprising accuracy.
If burning wakes you at night or is worse when you lie down, elevating the head of your bed by 15 to 20 centimetres reduces nocturnal acid reflux significantly. Using extra pillows under your head alone is less effective than raising the entire head end of the mattress — the angle needs to start at your waist, not your neck. Wedge pillows designed specifically for reflux achieve the same result more comfortably.
When Home Remedies Are Not Enough
Most stomach burning is straightforward and responds well to the remedies above. But some burning is a signal of something that needs proper medical attention, not another glass of milk.
Burning that occurs more than twice a week and does not respond to antacids. Difficulty swallowing, or food feeling stuck in your throat. Unexplained weight loss alongside the burning. Black, dark, or tarry stools — this can indicate bleeding in the digestive tract. Persistent vomiting. Chest pain that spreads to your arm, jaw, or back — this can indicate a cardiac problem, not stomach burning. Burning that began after starting a new medication, particularly NSAIDs, antibiotics, or bisphosphonates. Symptoms in anyone over 55 who has not had acid reflux investigated before.
Chronic burning that is properly investigated can usually be managed effectively with prescription proton pump inhibitors, treatment for H. pylori if that is the cause, or other targeted therapies. The difference between managing a symptom indefinitely and actually treating the cause often comes down to getting a proper diagnosis rather than relying on antacids permanently.
If you want a deeper look at causes and treatment options, Franciscan Health’s reviewed guide on heartburn home remedies covers the evidence behind each approach clearly, including which ones are worth trying and which carry more caveats than most sites admit.
Frequently Asked Questions
The fastest home options are a glass of cold milk sipped slowly, half a teaspoon of baking soda dissolved in water, or an over-the-counter antacid. Sitting or standing upright immediately also helps by keeping acid where it belongs. Cold water, ginger tea, coconut water, and a ripe banana are gentler alternatives that typically work within 15 to 30 minutes. Stop eating and avoid lying down until the burning passes.
The most common causes are acid reflux (stomach acid flowing back into the oesophagus), indigestion from eating too quickly or too much, spicy or fatty foods irritating the stomach lining, and stress increasing acid production. Less common causes include gastritis, peptic ulcers, and H. pylori bacterial infection. When acid reflux occurs regularly — more than twice a week — it is classified as GERD and warrants medical assessment.
Baking soda (sodium bicarbonate) is a quick natural antacid that neutralises stomach acid effectively and is safe for occasional use. Mix half a teaspoon in a full glass of water and drink it slowly. It should not be used daily — excessive use raises sodium levels and can cause side effects including gas and bloating. Avoid it if you are on a low-sodium diet, have kidney problems, or are pregnant without medical guidance.
Yes, for most people. The calcium in milk neutralises stomach acid and the cold temperature soothes the stomach lining. Sip it slowly rather than drinking it all at once. Low-fat or skimmed milk tends to work better for acid reflux than whole milk — the fat content in whole milk can slow gastric emptying, which may prolong symptoms for some people even while providing initial relief.
See a doctor if burning occurs more than twice a week, if it persists for more than a week despite home treatment, or if it comes with any of these warning signs: difficulty swallowing, unexplained weight loss, black or tarry stools, persistent vomiting, or chest pain that spreads to the arm or jaw. Also seek medical advice if burning started after beginning a new medication, or if you are over 55 and have not had reflux investigated before.
Yes, directly. The gut-brain axis is well-documented — stress increases stomach acid secretion, slows digestion, and can trigger inflammation in the stomach lining. Many people who experience burning during high-stress periods have no other underlying condition. Addressing the stress itself through slower eating, deep breathing, and reducing anxiety can reduce or eliminate stress-related burning without any medication needed.
Medical Disclaimer: This article is for informational purposes only and does not substitute professional medical advice, diagnosis, or treatment. Remedies described are for occasional, mild symptoms. If you experience frequent, severe, or worsening stomach burning, consult a qualified healthcare provider. Information is sourced from Medical News Today and Franciscan Health.
Disclaimer: WellbeingDrive provides health information for educational purposes only. Do not use this content as a substitute for professional medical advice. Consult your doctor before making health related decisions.

