Healthcare still trails behind sectors like media, finance, insurance, and retail when it comes to digital adoption. While most major industries have fully embraced digital transformation, medicine continues to move at a more cautious pace. Even so, progress is undeniable—around 75% of hospitals now use electronic health record systems. This contrast creates a fascinating tension: healthcare remains conservative in structure, yet increasingly dependent on technology. For medical education, that tension brings both serious challenges and powerful opportunities.
At the same time, digital breakthroughs are reshaping how future doctors learn. AI-driven tools, data platforms, and smart simulations are changing training models, introducing personalized learning paths and improving diagnostic accuracy before students even step into clinical practice. As healthcare systems grow more tech-centered, medical schools must evolve just as quickly. Preparing tomorrow’s physicians no longer means teaching medicine alone—it means teaching medicine within a deeply digital clinical environment.
This piece explores how leading medical institutions are adapting to this shift, using digital training to prepare graduates for the realities of modern healthcare.
The Digital Backbone of Modern Clinical Training
Digital solutions can uniquely solve the efficiency challenges that modern medical education faces today. Clinical programs need better infrastructure to match the fast-paced changes in healthcare delivery and education.
Why coordination challenges slow down clinical programs
Healthcare costs depend heavily on clinical efficiency, especially in value-based care settings. Administrative tasks create major bottlenecks—nearly 84% of healthcare leaders cite clinical documentation and coding as burdensome. More than half of U.S. providers show burnout symptoms, which hurts both their well-being and patient outcomes.
Money lost to these issues adds up fast. U.S. healthcare spending reaches about USD 4 trillion each year, with administrative costs eating up roughly 25%. Clinical education programs face these same coordination hurdles when they try to track student progress across multiple training sites.
Centralized platforms that line up schools, students, and instructors
Leading medical schools no longer rely on disconnected spreadsheets and manual oversight. Instead, they build unified digital ecosystems that bring students, faculty, and administrators onto the same platform. In many cases, this includes adopting advanced student clinical placement software that streamlines how institutions manage rotations, documentation, and competency tracking from day one.
These integrated systems allow schools to centralize requirement tracking, certifications, immunization records, and essential documentation without constant back-and-forth emails. They also support detailed curriculum mapping aligned with competency-based education models, ensuring that every clinical experience directly supports measurable learning outcomes. On top of that, built-in performance analytics help educators identify learning gaps early and refine curricula based on real-time data instead of assumptions.
For example, platforms like eMedley provide a comprehensive framework for monitoring student progress through case logging, skill validation, and time tracking across rotations. Similarly, CORE ELMS focuses on optimizing clinical rotation management with tools designed specifically for UME administrators, students, and preceptors. Together, these systems demonstrate how centralized digital infrastructure strengthens coordination, accountability, and educational quality.
Turning compliance and hour tracking into automated workflows
Healthcare institutions must follow 629 different regulations, which costs nearly USD 7.60 million yearly. Automation has become crucial—the 2022 CAQH Index shows that automation and optimized processes cut healthcare system costs by USD 187 billion annually.
Medical education uses automation to turn time-consuming tasks like preceptor evaluations and clinical hour tracking into efficient workflows. Harvard Medical School students now track clinical experiences through mobile apps in real-time instead of after-the-fact reporting.
These digital solutions free up valuable time for faculty and students. A medical educator put it best: this technology “can free up some of that time so we can devote it to what we’re really here for, which is helping people”.
Core Components Top Medical Schools Include in Digital Healthcare Curricula
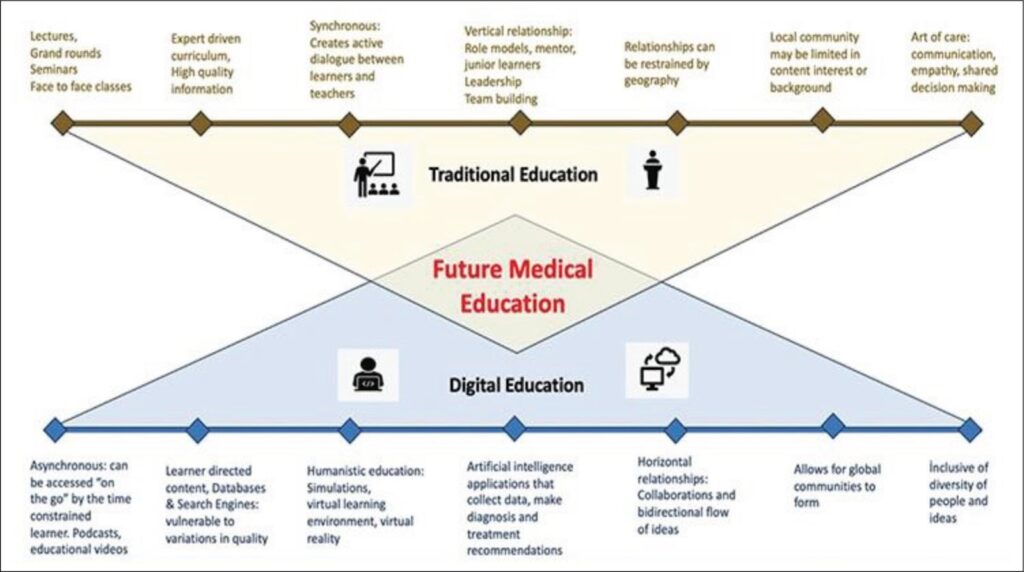
Medical schools now focus on key digital elements in their programs to get future doctors ready for tech-driven healthcare. Students need these skills to work in modern clinical practice.
AI-Powered Clinical Simulation and Virtual Patients
AI helps boost medical education by creating individual learning paths based on each student’s performance. This approach helps students learn better and stay involved. Students can practice taking patient histories, making diagnoses, and planning treatments safely with virtual patients. These AI-powered virtual patients copy real-life conditions and give live feedback based on student choices. The results speak for themselves – the AIPatient system scored 94.15% accuracy when answering medical questions from Electronic Health Records. Students also found social robotic platforms better than regular computer programs.
Electronic Health Records and Health Information Systems Training
Students must learn basic biomedical informatics skills about health information technology. They need to understand electronic medical record systems and how these systems keep patients safe. Doctors spend most of their day working with EHRs, but many students don’t get enough training. Programs like the Regenstrief Teaching Electronic Medical Record (tEMR) help solve this issue. Students can work with over 12,000 de-identified patient records to learn how to use records, document visits, and write orders.
Telemedicine and Remote Care Delivery Skills
A detailed telemedicine program usually covers five main areas:
- Introduction to telehealth fundamentals
- Telehealth encounter techniques
- Legal and technical requirements
- Access and equity considerations
- Future developments and applications
Students attend lectures, watch telehealth doctors work, and practice video visits with trained patient actors to learn virtual examination skills. Right now, more than 60 allopathic medical schools include some type of telemedicine training in their clinical rotations.
Data Analytics and Clinical Decision Support Tools
By 2017, most healthcare facilities had adopted electronic health records with decision support features – over 90% of hospitals and 80% of clinics. These systems help prevent mistakes and support various care tasks. Medical schools now teach students about these tools so they understand how data improves clinical decisions and patient care.
How Leading Institutions Integrate Digital Innovation in Healthcare Training

Top educational institutions are creating trailblazing solutions through detailed approaches to digital health training. Students now prepare themselves for a technology-driven future in healthcare.
Embedding Technology Across All Years of Study
Medical schools introduce digital concepts from day one. Harvard Medical School has created a one-month introductory course on AI in healthcare for all incoming students on the Health Sciences and Technology track. “I don’t know of any other med school doing that, definitely not in the first month,” notes one faculty member. This helps “ground students in the idea that medicine is going to be different going forward”. Students’ attention is drawn to specialized tracks like Harvard’s AI in Medicine PhD program, which received over 400 applications for just seven spots.
Hands-On Practice with Real Healthcare Digital Tools
Real-life experience with actual technologies serves as the lifeblood of effective digital training. Students showed remarkable progress after hands-on laboratory sessions. The data reveals 75.51% reported better confidence in training patients to use wireless monitoring devices.
Students start with tools ranging from EHR platforms using de-identified patient data to virtual reality simulations that let them experience patients’ environments firsthand. They advance to working with specialized equipment like endoscopes, 3D printers for custom medical devices, and telehealth robots.
Collaboration Between Medical and Technology Departments
Programs break traditional academic barriers. A student chosen from nearly 1,600 applicants across 88 countries joined a global healthcare hackathon. The student noted that “by using technology we can unlock so much untapped potential”. Medical schools develop innovative teaching tools like virtual dissection tables that make use of information from 3D anatomical visualization to boost comprehension and involvement. Hospitals affiliated with medical schools integrate AI into their clinical workflows and create natural opportunities for cross-disciplinary learning.
Continuous Faculty Development in Digital Health
Faculty preparedness poses a significant challenge—less than 30% of healthcare professionals report feeling sufficiently prepared to use existing digital health tools effectively. Institutions address this through structured training programs and resources. Medical schools create policies and guidelines for both students and faculty regarding AI use. They conduct targeted training sessions for course and clerkship directors. Evidence shows faculty members gain more confidence and develop favorable attitudes toward integration after structured AI training.
Assessment Methods for Digital Competencies
Digital competencies need standardized evaluation approaches. The Digital Health Competencies framework divides skills into four domains: professionalism in digital health, patient and population digital health, health information systems, and health data science. Assessment involves scenario-based challenges instead of traditional testing. One confirmed model gives professionals clinical scenarios with 28 questions to answer within 60 minutes. Another model uses exploratory factor analysis to identify two key factors: Digital Interaction & Responsibility and Digital Content Development and Software Mastery.
Overcoming Implementation Challenges in Digitalization in Healthcare Education
Healthcare education institutions face many barriers when implementing innovative digital solutions. They need well-laid-out planning and systematic approaches to overcome these obstacles.
Addressing Limited Technical Infrastructure and Resources
Poor broadband connectivity and limited access to digital devices affect marginalized communities the most. Medical schools must build resilient infrastructure to bridge this digital divide. They should focus on mutually beneficial alliances that help share experiences and resources among institutions.
Managing Faculty Resistance and Knowledge Gaps
Many faculty members see digital tools as a burden and don’t feel confident about their digital skills. Learning technology experts who could help are often seen as subordinates instead of equal partners in education. In spite of that, research shows that faculty members become more confident and positive about using technology after structured AI training.
Balancing Digital Skills with Clinical Fundamentals
The medical curriculum is already packed, so educators must carefully choose the most important digital health skills to teach. The quickest way to teach is to focus on basic principles and broader views of digital health rather than specific applications.
Ensuring Equal Access for All Students
People in low-income areas, elderly communities, and rural regions with limited internet access find it hard to adopt digital tools. Schools should offer different ways to access resources and complete training to help everyone become tech-savvy.
Privacy and Ethics in Digital Health Training
Students must learn about data security, rules like HIPAA and GDPR, and how biased algorithms can affect healthcare decisions. Ethics training should stress the importance of informed consent and clear communication in digital settings.
Conclusion
Healthcare education stands at a decisive turning point. Medical schools now recognize that preparing future physicians means equipping them for a technology-driven clinical world, not just traditional practice. Centralized learning platforms, AI-powered simulations, EHR training, and telemedicine skills form the backbone of modern curricula. Institutions that integrate technology across study years and encourage cross-department collaboration provide practical models others can follow as they modernize their programs.
Still, meaningful challenges remain. Faculty hesitation, limited infrastructure, crowded curricula, and unequal access risk widening the digital divide in medical training. Thoughtful program design must balance technical fluency with clinical fundamentals and human connection. The most successful schools emphasize adaptability, ethical awareness, and critical thinking about emerging tools. By combining technological competence with compassionate care, medical education can produce physicians ready for an evolving healthcare landscape.
Disclaimer: The content on Wellbeingdrive is for informational purposes only and not a substitute for professional advice. Always consult a qualified expert for health concerns.

